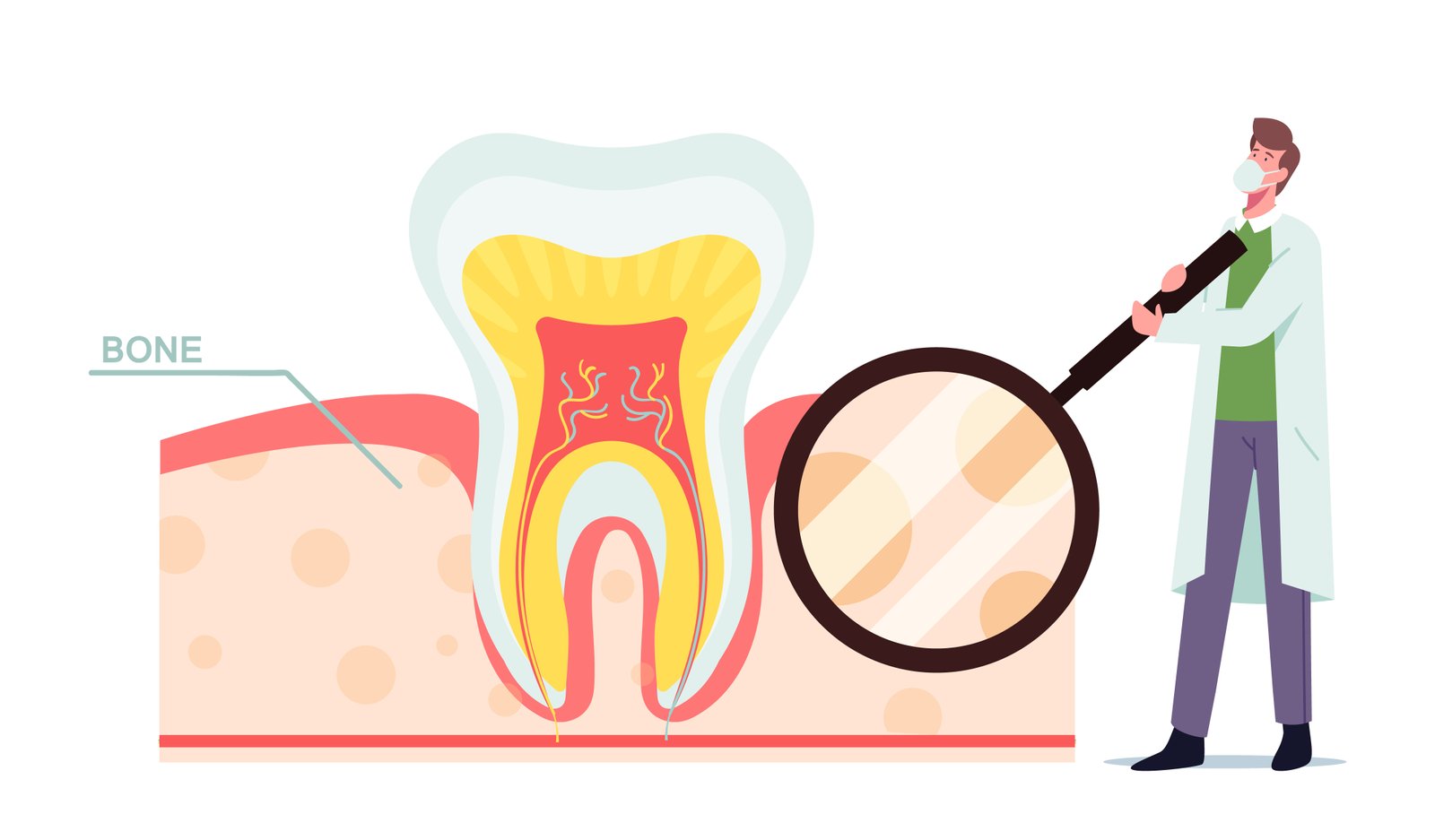
Periodontal disease is characterized by inflammation and infection of the gums and the bone that supports your teeth. Poor hygiene may be the cause, but certain individuals are more vulnerable to this kind of infection.
Possible symptoms include loose teeth, swollen and bleeding gums, and bad breath. Various therapies are available based on the severity of the illness.
Overview
What is periodontal disease?
The phrase "gum disease," also referred to as "periodontitis," describes an infection and inflammation of the tissues surrounding your teeth.
Bad oral hygiene has the potential to cause gum disease. Nevertheless, some people are more prone to this issue than others, even with proper brushing and flossing.
How common is periodontal disease?
In the US, about half of adult adults suffer from gum disease. It is the main factor in tooth loss.
Symptoms and Causes
What are the symptoms of periodontal disease?
Symptoms of periodontal disease could include:
-
Reddish or purplish gums.
-
Bleeding.
-
Soreness.
-
Bad breath (halitosis).
-
Unpleasant taste.
-
Pain when chewing.
-
Gum recession (receding gums from your teeth).
-
Loose teeth.
-
A modification to the fit of your teeth.
Periodontal disease stages
Healthy gums are firm to the touch. They neither bulge nor bleed. However, bleeding, swelling, and stained (reddish or purplish) gums might be a symptom of periodontal disease. If gum disease is not addressed, it can lead to the destruction of your jawbone and eventual loss of your teeth.
The tissues surrounding your teeth eventually deteriorate. Actually, most people who have gum disease don't experience any pain, especially while it's first developing. Thus, it's critical to recognize the warning indicators.
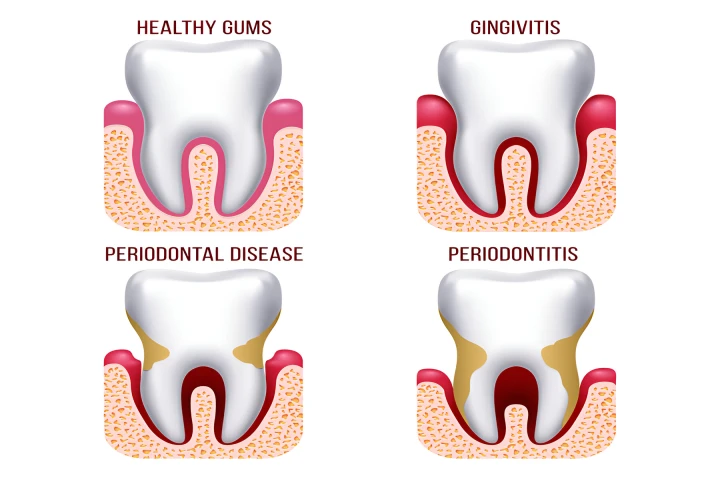
Gum disease progresses in four stages:
-
Gingivitis represents the initial phase of gum disease. Initially, it may bleed from red, puffy gums when you brush or floss. There isn't any bone loss at this point. Gingivitis is therefore completely curable with the right care.
-
Mild periodontitis: Your gums have allowed the bacteria to penetrate and damage the underlying bone. Your gums may become separated from your teeth and develop pockets surrounding them. Plaque and germs like to lurk in these pockets, where your toothbrush and floss can't get to them.
-
Moderate periodontitis: The ligaments, soft tissues, and bone that support your teeth in place start to deteriorate if you don't treat bacteria. Bad breath and pus (an infection) near your gum line are possible symptoms. At this point, some people start to feel pain.
-
Advanced periodontitis: As the illness advances, bone loss continues. Your teeth may get loose as a result and finally fall out.
Gum disease is reversible if caught early enough. If you have already lost bone surrounding your teeth due to infection, the sickness is too advanced to be corrected. On the other hand, with appropriate care and regular, conscientious oral hygiene, you can control it.
What causes periodontal disease?
The primary cause of periodontal disease is the accumulation of dental plaque. Numerous types of bacteria found in plaque have the ability to infect your gums.
That's why having bad dental hygiene increases your risk of developing gum disease. Because genes alter how the immune system reacts to bacteria, they can contribute to gum disease in some individuals.
Gum disease risk factors
Anything that raises your chances of contracting an illness or condition is called a risk factor. The following are some possible risk factors for periodontal disease:
-
Smoking or other tobacco use.
-
Poor oral hygiene.
-
Autoimmune conditions, such as crohn's disease, scleroderma, and lupus.
-
Changes in hormones, especially during menopause, pregnancy, and puberty.
-
Stress.
-
Genetics: If your parents, grandparents, or siblings have gum disease, your chances of developing it are higher.
Is periodontal disease contagious?
Gum disease-causing bacteria can spread from person to person. Although short-term, casual contact cannot transmit gum disease, prolonged, frequent salivary contact (such as kissing) can raise your chance of developing periodontal disease.
What are the complications of periodontal disease?
Gum disease deteriorates further without therapy, seriously harming your oral health. It causes an infection that spirals out of control and may result in tooth loss.
Additionally, studies have demonstrated the direct connection between gum disease and general health and wellbeing. Gum disease has been related to heart disease, stroke, and diabetes, among other health problems.
Diagnosis and Tests
How do dentists diagnose periodontal disease?
If you have gum disease, a dentist can detect it during a standard examination. They will examine your teeth for plaque accumulation and inquire about your symptoms. They could suggest that you see a periodontist (a specialist in gums) for additional assessment and care.
A periodontal probe is a tool that a dentist or periodontist uses to measure the pockets surrounding your teeth. This indicates to them the amount of bone loss surrounding your teeth. Your gum disease is more serious the deeper the pockets are.
Your periodontist will examine your bite, the degree of tooth sensitivity, and the extent to which your gums are receding (separating from your teeth).
They will also take dental X-rays. The areas of bone loss are clearly visible in these pictures. In order to see how your bone has altered over time, they can also examine previous X-rays.
Management and Treatment
Is periodontal disease curable?
Although gum disease cannot be cured, it can be controlled with the right care. You can't treat it because, in most cases, the structural support surrounding your teeth doesn't grow back completely. On the other hand, periodontal therapy can lessen infection and partially restore your bone and tissue.
Genetics is another factor. Oral bacteria are diverse in their nature. Simply put, some people are more likely to have the kind that leads to gum disease.
Gingivitis, or very early periodontal disease, is one stage of gum disease that is completely reversible. Gingivitis can be reversed with consistent dental cleanings and careful oral hygiene if caught early enough.
How is periodontal disease treated?
There are numerous options for treating periodontal disease. The one that is best for you will rely on several aspects, such as the severity of your ailment, among others.
-
Your health.
-
Whether you smoke.
-
What treatments you’ve had in the past.
Dental cleaning and improved oral hygiene
With regular dental cleanings and better oral hygiene, those with very early periodontal disease (gingivitis) may be able to reverse the illness. This cautious therapy eliminates harmful oral bacteria before the disease has a chance to worsen because there isn't yet any bone loss.
Brushing and flossing twice or three times a day, as well as routine dental checkups and cleanings, are all part of good oral hygiene.
Scaling and root planing
Regular dental cleaning is comparable to scaling and root planing. However, it cleans below your gum line, where your toothbrush and floss can't reach, getting rid of bacteria and plaque. For patients with minor gum disease, periodontists advise this course of treatment.
A dental hygienist removes plaque from your teeth by scaling them and smoothing the surfaces of your roots with planes to prevent bacteria from adhering again. Using local anesthetic, the treatment is typically completed in two visits or less.
Pocket reduction surgery
Pocket reduction surgery, also known as osseous surgery, may be necessary for patients with moderate to advanced gum disease. The aim is to get rid of tartar and plaque that are buried behind your gums so deeply that your hygienist is unable to reach them.
A periodontist makes an incision (cut) in your gums and forms a flap during this treatment. This enables them to temporarily separate your gums from the roots of your teeth.
They will next smooth out any rough spots and remove germs, tartar, and plaque from the roots of your teeth. When finished, they will use stitches to close the incision and realign your gums.
Periodontists frequently mix guided tissue regeneration, gum grafting, bone grafting, and pocket reduction surgery with other regenerative techniques.
LANAP (Laser-assisted new attachment procedure)
Additionally, certain periodontists provide LANAP pocket reduction. With this surgery, a portable laser is used to treat periodontitis. The laser preserves healthy gum tissue while focusing on unhealthy gum tissue.
A less intrusive option to conventional pocket reduction surgery is LANAP. However, the outcomes are not all that consistent.
Bone grafting
To restore bone that you've lost to gum disease, a periodontist may employ a dental bone graft. Following the removal of the infection, the places where the bone has deteriorated will be filled up with bone grafting material. This substance serves as a space-holder or scaffold, allowing your body to gradually regenerate new bone.
Gum grafting
Your dentist might suggest tissue grafting, commonly known as gum transplant surgery, if you have lost gum tissue due to periodontal disease. This process thickens your gum line and hides any exposed tooth roots.
A periodontist will add tissue to the gum recession areas during this surgery. This tissue can originate from the roof of your mouth, or it might be acquired by your healthcare professional from an authorized bone and tissue bank.
Guided tissue regeneration (GTR)
Periodontists typically combine a bone graft with directed tissue regeneration. GTR stops soft tissue from forming in periodontal deficiencies, which are regions of broken down bone, and aids in their restoration.
An artificial membrane is positioned by a periodontist between your gums and the freshly inserted bone grafting material during GTR. The membrane maintains that gap open so that new bone can grow there in place of the soft tissue since soft tissue regenerates more quickly than bone.
Platelet-rich fibrin (PRF) and platelet-rich plasma (PRP)
Growth factors found in platelet-rich fibrin (PRF) and platelet-rich plasma (PRP) hasten tissue regeneration and repair. PRF and PRP can be extracted from a little blood sample by a periodontist.
To separate the plasma from your red blood cells, they will spin the sample in a centrifuge, a lab device that spins quickly using centrifugal force. After that, the surgical site will receive fibrin or platelet-rich plasma.
This kind of therapy not only promotes healing but also speeds up recovery and lessens discomfort after surgery. It's also totally safe because it originates from your own blood.
Prevention
Can I prevent periodontal disease?
Yes, with regular and appropriate dental hygiene, gum disease can be avoided in most cases. Some people have a hereditary predisposition to gum disease, or they may have other health issues. You might require more frequent cleanings from your dental hygienist in these situations.
How may the risk of periodontal disease be reduced?
In order to lower your gum disease risk:
-
Every day, brush your teeth two to three times.
-
Every day, floss between your teeth.
-
Put some antimicrobial mouthwash on.
-
Steer clear of tobacco usage, including smoking.
-
See your dentist for routine examinations and cleanings.
Outlook / Prognosis
What’s the outlook for people with periodontal disease?
Periodontal disease does not pose a threat to life. However, it can result in other medical disorders that could need to be treated, particularly if the infection spreads to other body parts.
Gum disease has no known cure. However, it may be controlled with the right care. Early gum disease diagnosis and treatment might help you take better care of your oral health.
Living With
When should I see a dentist?
See a dentist right away if your gums start to bleed, become painful, or swell. The key is early detection. Your dentist will recommend you to a periodontist if you require treatment beyond a simple cleaning.
What questions should I ask my periodontist?
Here are some questions you might want to ask your periodontist if you have gum disease:
-
What is the stage of my gum disease?
-
Will I require nonsurgical or surgical care?
-
Do you provide choices for sedation dentistry?
-
How much time will it take to recover?
-
When can I resume my job or studies?
-
How frequently should I get my teeth cleaned?
Additional Common Questions
What does gum disease look like?
Gums that are swollen, sensitive, and reddish or purplish are early indicators of gum disease. There can be a plaque accumulation on your teeth. You can have pus around your gum line and loose teeth as the disease progresses.
How long after developing periodontal disease can you keep your teeth?
The severity of your ailment determines this. Due to the fact that each person is unique, there is no hard and fast rule. Generally speaking, your chances of losing teeth decrease with the early treatment of gum disease.
A note from PondStories
Most of the time, especially in the early stages, periodontal disease is painless. It's critical to recognize the warning indicators so that you can receive the right care before the illness gets worse. Gum disease can negatively impact both your oral and general health if left untreated. Your chance of developing heart disease, stroke, and diabetes increases as the infection spreads to other parts of your body and other parts of your mouth. Inform your dentist if you have bleeding, sore, or swollen gums. They can assist you in eliminating infection and returning to gum and tooth health.